Resuming Elective Surgery in 2021: Cutting Through the Backlog and the Road to Recovery
By: John Mehall, MD
A Backlog of 1,000,000+ Surgical Procedures and $200B in Financial Losses
On March 18, 2020, the Centers for Medicare and Medicaid Services (CMS) released guidelines recommending postponing or cancelling elective, non-essential medical, surgical, and dental procedures to preserve resources for treating COVID-19 patients. The guidance was advisory rather than mandatory and did not define “elective and non-essential,” which left local authorities on their own to decide which services should be curtailed. By mid-April 36 states and Washington DC had developed some form of response. This ranged from detailed lists of proscribed services to simple statements that non-urgent procedures should be postponed until further notice. Fourteen states left decisions on who should or should not get care up to individual providers.
Compounding the impact of the CMS guidance were state shelter-at-home mandates. By April 15, 42 states and the District of Columbia had issued such mandates. The combination of the two policies had a profound impact on the delivery of routine services and elective surgery. Outpatient visits plummeted from February to the end of March by nearly 60 percent. Over 4 million operations were cancelled from March to June, costing healthcare institutions an estimated $200 billion in financial losses.

This ban, along with intermittent pauses to elective procedures due to fluctuations of COVID-19 and health systems’ diminished bed capacity, has led to an unprecedented surgical backlog. A recent study predicts that the post-pandemic backlog will exceed one million cases for spinal fusions and joint replacement in orthopedic surgery by 2022, and the Journal of Cataract & Refractive Surgery estimates a backlog of 1.1-1.6 million cataract surgeries during that same time.
By the end of 2020, it’s been reported that two months or more of pent up excess surgical demand may have accumulated. Consulting firm McKinsey states that in order for the United States to work through this backlog in less than a year, it would require hospitals to operate at 120% of historical volumes. However, given challenges around workforce shortages, inpatient bed availability, and operating room (OR) capacity, a more realistic scenario is operating at a 10% increase above baseline volumes. This would result in a much longer, 20-month timeline to work through these cases.
Looking Forward: Jumpstarting Elective Surgeries
With the increasing distribution of the COVID-19 vaccine and the majority of states lifting restrictions on elective surgery, hospitals across the United States have been trying to understand how to effectively implement strategies to ramp up surgical volume. Given the growing backlog and the financial toll these cancellations have had on the bottom line, there may be temptation to ramp up quickly while shortcutting a thoughtful strategy.
Doing so may lead to many negative consequences – poorly thought out policies for distributing resources across elective surgical cases can generate unintended bottlenecks that may impede operations. Similarly, not prioritizing equitable access when building out a strategy may inadvertently reinforce disparities in health equity by favoring patients from higher socioeconomic backgrounds.
There is a short window right now in which our hospitals and health systems must take a data-driven approach to prioritize this pent-up demand. And develop a strategy for addressing it quickly and efficiently.
Hospital executives and surgeons must determine which factors that they must prioritize against.
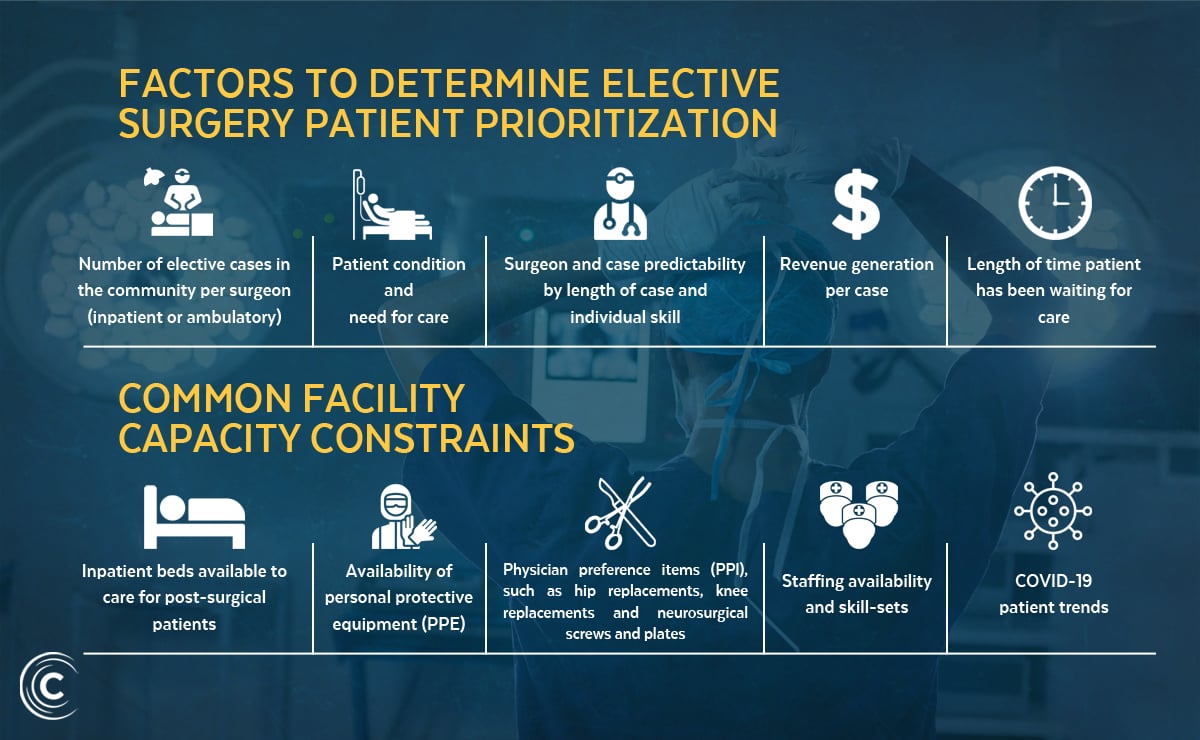
Organizations will have to rethink their traditional models in favor of a rapid-response mentality. You can’t resume a business-as-usual approach where hospitals try and fit the pent-up demand into their current scheduling operations. That won’t work, and it will lead to capacity constraints.
Current levels of operational inefficiency, especially around traditional block schedule management, will get in the way of meeting both normal and pent-up demand. It doesn’t allow for the prioritization approach to succeed.
Five Strategies to Resume Elective Surgery in 2021
Tackling the backlog in an efficient and effective manner while minimizing COVID-19 risks will require thorough planning, coordination and the development of a systematic and structured approach. In our new eBook, “Resuming Elective Surgery in 2021”, we go in-depth and recommend five strategies that healthcare leaders can implement to meet their clinical objectives and develop better operational efficiency to address their institution’s backlog.
About Curative Talent
Recently acquired by Doximity, the world’s largest medical network, the all-new Curative is a healthcare recruiting and staffing agency that finds incredible talent with less hassle using better data. We combine the industry-leading expertise and deep relationships of our experienced recruiters with Doximity’s intelligent technology to fill roles quickly and effectively.
Our unique algorithm matches the right candidates for the right jobs; leveraging our unique relationship with Doximity, we’re able to reach candidates that no one else has access to. To learn more about how we can help your facility address your hiring needs through our fresh, differentiated approach to healthcare recruiting and staffing, please visit https://curativetalent.com/.

